Tiny Bursa Balloons to Bursitis
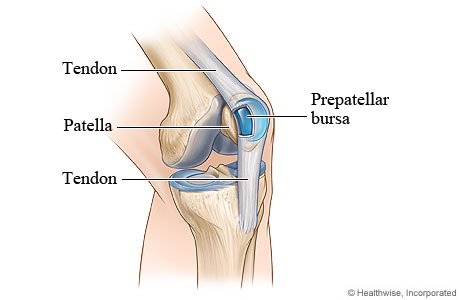
A bursa is a thin, fluid-filled sac that cushions and lubricates between bone and surrounding soft tissue, such as skin, muscles, ligaments, and tendons. It’s like a tiny water balloon with only a few drops of fluid wedged between two surfaces. An adult body contains about 160 bursae with 11 around the knee joint. When inflamed, a bursa’s thin lining thickens and the bursa fills with more fluid, which can swell to a grapefruit-sized lump under the skin and cause tenderness and pain. Any bursa in the knee can become inflamed, but prepatellar bursae on the front of the knee are especially susceptible to bursitis. Bursitis can be caused by trauma to the knee. Swelling and other symptoms may appear within 24 hours, similar to a bruise. Bursitis is also caused by mini-traumas, such as repeated kneeling at work or sports. Mini-trauma symptoms may appear slowly, over several days or weeks.
If one or both bursae in the front of the knee become swollen and inflamed, a lump the size of a grapefruit can balloon under the skin called knee bursitis. If accompanied by a fever, go to DOC immediately.
A DOC guest who had ankle surgery after a serious fall developed bursitis. She was using a steerable knee scooter. It is a great option for getting around when a person is non-weight-bearing on one leg. However, the injured leg is always bent when using the scooter. This particular guest was steering it through Costco, malls and her city sidewalks. Her knee was continuously bent during these excursions. The constant bent knee on the scooter was the same as repeated kneeling and she developed min-trauma bursitis. When she reduced the scooter trips and long adventures with a bent knee, the mini-trauma bursitis subsided. The DOC orthopedic specialist must rule out other knee problems, such as arthritis, gout, tendonitis, fracture, or tumor, before making a diagnosis of prepatellar bursitis or knee bursitis. X-rays provide clear pictures of the bone to check for a fracture. CT scan, MRI, or ultrasound images may be ordered to check for other soft tissue injuries. The DOC orthopedist will discuss symptoms, inspect the affected knee, palpate for tenderness, and assess the range of motion. If an infection is suspected, the bursa may be aspirated and sent to the lab for analysis. Septic knee bursitis requires antibiotic treatment and monitoring. Controlling inflammation of the bursa is the main treatment goal. Rest, cold compresses 20 minutes two or three times a day, elevated knee, a compression bandage, and anti-inflammatory medications may help to alleviate symptoms and decrease swelling. It the swelling and pain do not respond to these measures, the DOC surgeon may decide to drain or aspirate the bursa with a needle and inject a corticosteroid medication. Then if the swelling continues, the surgeon may recommend surgical removal of the bursa. To learn about other knee injuries treated by DOC, visit our conditions page here.
For more information on the cost of care, click here.




